3D Automated Whole Breast Ultrasound (ABUS)
Know Your Body. Understand Your Options.
Are you dense?
Dense breasts are normal; up to 40% of American women have them. It simply means that you have more fibrous, glandular breast tissue in your breasts than fatty tissue. Younger women typically have denser breast tissue. As women age, and especially after menopause, their breast tissue becomes less dense. If they take postmenopausal hormones, their breasts may remain dense.
Breast density is measured during your annual screening mammogram
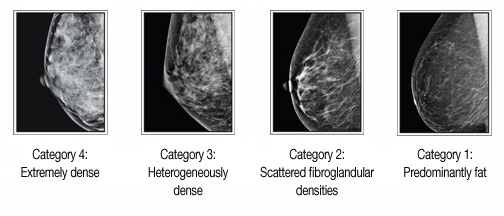
All mammography reports from our center contain a classification of breast density based on the Breast Imaging-Reporting and Data System (BI-RADS) breast composition categories:
Why is breast density important?
While the reasons are not yet fully understood, women with denser breasts are at an increased risk for breast cancer. In addition, clinical studies have shown that women with dense breasts can benefit from a supplemental form of screening in addition to mammography.
Supplemental screening
For women classified as BI-RADS 3 (heterogeneously dense) and BI-RADS 4 (extremely dense). Supplemental screenings can include breast MRI and 3D Automated Whole Breast Ultrasound (ABUS).
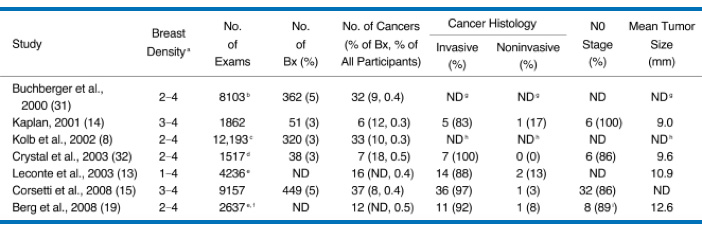
Breast MRI is generally recommended for women who are determined to be at high risk for breast cancer (e.g. another family member was diagnosed with the disease). For most women ABUS is a less expensive and highly accurate form of screening. The Invenia™ ABUS used at Desert Rose Women’s Center has been clinically proven to improve breast cancer detection by 35.7% over mammography alone, and is especially useful at detecting smaller and earlier stage cancers in women with dense breasts.
Why haven’t I heard of breast density before?
The issue of breast density has only recently emerged into the national spotlight, and the majority of clinical research on the subject is less than ten years old. Just seventeen states have breast density notification laws, but that number is growing. While New Mexico does not have such a law in place as of yet, we at Desert Rose Women’s Center feel strongly that this is an important issue that both doctors and patients need to know about.
The clinical evidence is clear, and this is not a medical “fad.” Breast density is not only a risk factor for breast cancer, but it can also impact a woman’s ability to achieve early detection using traditional methods. It is widely agreed that early detection is the key to surviving breast cancer, so any issue that can impact a woman’s confidence in her healthcare strategy must be considered.
Learn the facts for yourself. Talk to your doctor. If you need more information, we are here to help.